How to Prescribe Patient-Centered Home Hemodialysis (HHD) in 3 Steps:
Clinical considerations for increased frequency
5+ Days Per Week
More Frequent During Waking Hours
- Improved blood pressure (BP) control & survival1-6
- Reduced left ventricular hypertrophy & cardiovascular hospitalizations2,5,6,7
- Reduced ultrafiltration rate (UFR), recovery time and hypotensive episodes2,3,7,8-13
- Improved sleep quality, restless leg syndrome & health-related quality of life3,14-16
More Frequent During Waking Hours
- Benefits from 5+ days per week (above) plus:
- Improved sleep and obstructive sleep apnea12,15,17
- Best dialytic phosphorus control2,18,19
- Increased reduction in post-dialysis recovery time13
Every Other Day
- Mitigates the 2-day gap20
- May enable decreased ultrafiltration rate (UFR) by:2,8
- Increasing time per treatment
- Increasing number of treatments per week
3 Days Per Week
- Presents room for improvement
- Longer duration treatments (example: nocturnal) has improved mortality in observational studies1
Total weekly treatment time is driven by weekly patient fluid gains and ultrafiltration rate (UFR)
Clinical Considerations for Decreasing Target UFR
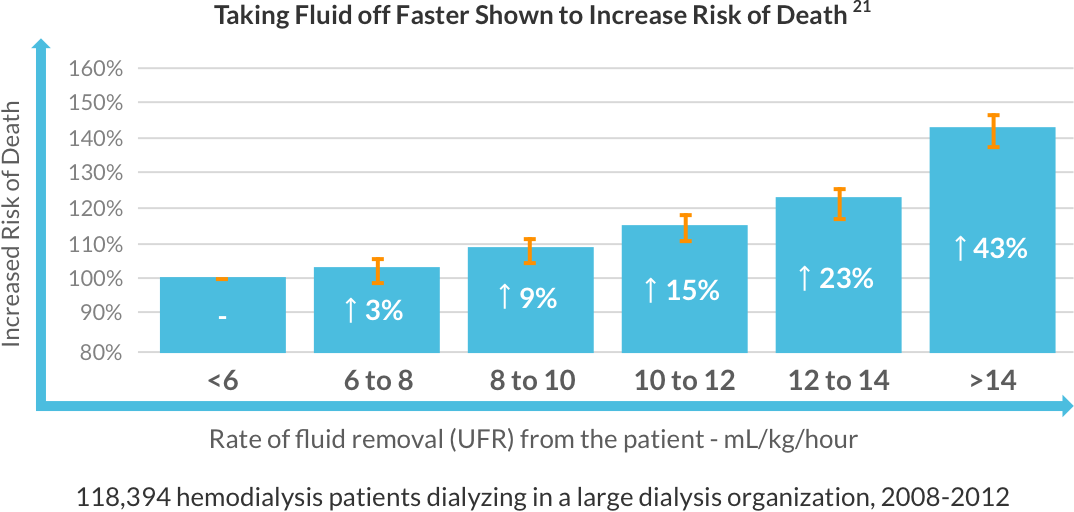
Ultrafiltration rates at or below 8mL/kg/hr suggest lower mortality risk.
Patients who perform HHD more frequently have an average UFR of 6.0 mL/kg/hour, and 14% of those patients have a UFR at or above 10mL/kg/hour.9
Patients who receive conventional thrice-weekly in-center HD have an average UFR of 9.5 mL/kg/hour, and 38% of those patients have a UFR at or above 10mL/kg/hour.9
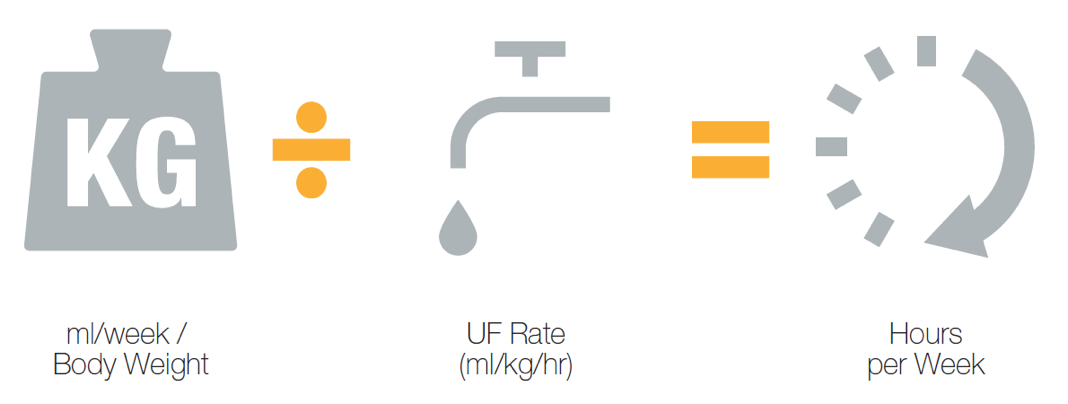
Calculating Treatment Time for Optimal Fluid Removal
To calculate the total treatment hours per week, start with the patient's weekly fluid gain in a given week, divided by the patient's weight.
Divide the weekly fluid needing to be removed by the ultrafiltration rate to calculate the total treatment time per week.
Total treatment time per week divided by the number of treatments per week is the number of hours per treatment.
Literature suggests a UFR of 6-8 mL/kg/hour, 5-6 treatments per week and a total of at least 12 hours of treatment per week. 15 hours of treatment per week is typical.1-22
Example: If a 80kg patient is putting on 9,600 mL of fluid per week, that must be removed. With a desired UF rate of 8mL/kg/h, the result is a treatment time of 15 hours per week.
Factors affecting dialysate treatment volume
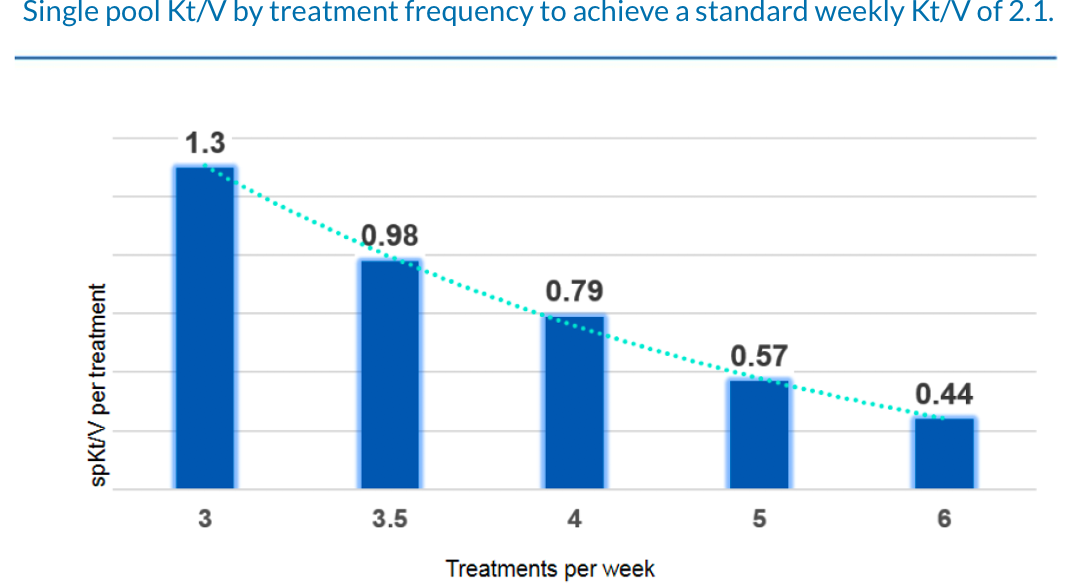
The per-treatment dialysate volume is determined by target Kt/V, total body water, frequency, duration and residual renal function. Kt/V, or urea clearance normalized to patient total body water, is the standard by which hemodialysis adequacy is measured and compared. A weekly standard Kt/V (stdKt/V) target dose can be translated into a per-treatment single pool Kt/V (spKt/V) for any given treatment regimen (frequency and duration). The spKt/V and the patient’s total body water determine the volume per treatment at which the dialysate is efficiently used.
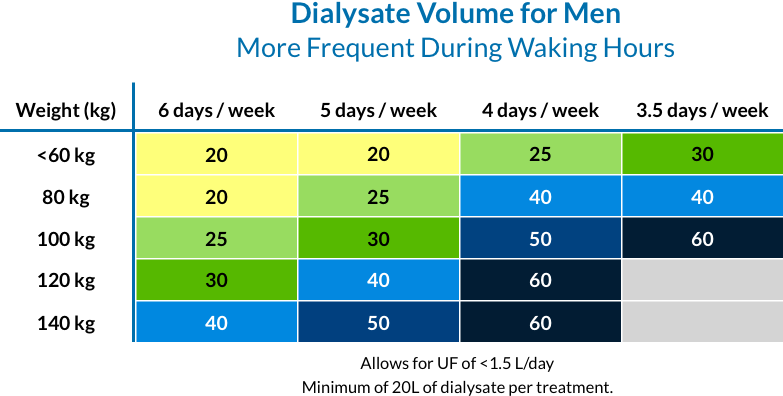
Recommended treatment volumes by gender, weight and frequency
Low volume dialysate treatments have improved small solute clearance and saturation when the dialysate flow rate is approximately 1/3 (or less) that of the blood flow rate. The following table is an example of estimated volume of dialysate needed to achieve a standard weekly Kt/V of 2.1 for men, assuming shorter treatments and a dialysate flow to blood flow ratio of 30% to 40%.
For additional guides, for both women and nocturnal treatments, download the Dialysate Volume Quick Reference Guide.
NxStage Dosing Calculator
Provides patient-specific therapy schedules based on scientific peer-reviewed formulas and journals.
Used for:
- Evaluating and discussing potential therapy options with new HHD patients
- Evaluating flexible therapy options as current HHD patients' needs change
Resources
NxStage is devoted to supporting healthcare professionals
Risks and Responsibilities
The reported benefits of home hemodialysis (HHD) may not be experienced by all patients.
The NxStage System is a prescription device and, like all medical devices, involves some risks. The risks associated with hemodialysis treatments in any environment include, but are not limited to, high blood pressure, fluid overload, low blood pressure, heart-related issues, and vascular access complications. When vascular access is exposed to more frequent use, infection of the site, and other access related complications may also be potential risks. The medical devices used in hemodialysis therapies may add additional risks including air entering the bloodstream, and blood loss due to clotting or accidental disconnection of the blood tubing set.
Home hemodialysis with the NxStage System during waking hours may not require a care partner, provided a physician and a qualified patient agree that solo home hemodialysis is appropriate. Patients performing nocturnal treatments are required to have a care partner. Care partners are trained on proper operation and how to get medical or technical help if needed.
Certain risks associated with hemodialysis treatment are increased when performing solo HHD because no one is present to help the patient respond to health emergencies. If patients experience needles coming out, blood loss, or very low blood pressure during solo HHD, they may lose consciousness or become physically unable to correct the health emergency. Losing consciousness or otherwise becoming impaired during any health emergency while alone could result in significant injury or death. Additional ancillary devices and training are required when performing solo HHD.
Certain risks associated with hemodialysis treatment are increased when performing nocturnal therapy due to the length of treatment time and because therapy is performed while the patient and care partner are sleeping. These risks include, but are not limited to, blood access disconnects and blood loss during sleep, blood clotting due to slower blood flow and/or increased treatment time, and delayed response to alarms when waking from sleep.
Patients should consult their doctor to understand the risks and responsibilities of performing these therapies using the NxStage System.
References
- Rivara MB et al. Extended-hours hemodialysis is associated with lower mortality risk in patients with end-stage renal disease. Kidney Int. 2016 Dec;90(6):1312-1320.
- FHN Trial Group, Chertow, G.M., Levin, N.W., Beck, G.J. et al. In-center hemodialysis six times per week versus three times per week. N Engl J Med. 2010; 363: 2287–2300.
- Morfin, J.A., Fluck, R.J., Weinhandl, E.D., Kansal, S., McCullough, P.A., and Komenda, P. Intensive hemodialysis and treatment complications and tolerability. Am J Kidney Dis. 2016; 68: S43–S50.
- Bakris, G.L., Burkart, J.M., Weinhandl, E.D., McCullough, P.A., and Kraus, M.A. Intensive hemodialysis, blood pressure, and antihypertensive medication use. Am J Kidney Dis. 2016; 68: S15–S23.
- Weinhandl ED, Gilbertson DT, Collins AJ. Mortality, Hospitalization, and Technique Failure in Daily Home Hemodialysis and Matched Peritoneal Dialysis Patients: A Matched Cohort Study. Am J Kidney Dis. 2016;67(1):98-110.
- Weinhandl, E.D., Liu, J., Gilbertson, D.T., Arneson, T.J., Collins, A.J. Survival in daily home hemodialysis and matched thrice-weekly in-center hemodialysis patients. J Am Soc Nephrol. 2012;23:895–904.
- McCullough, P.A., Chan, C.T., Weinhandl, E.D., Burkart, J.M., and Bakris, G.L. Intensive hemodialysis, left ventricular hypertrophy, and cardiovascular disease. Am J Kidney Dis. 2016; 68: S5–S14.
- Raimann, J.G., et al. The Effect of Increased Frequency of Hemodialysis on Volume-Related Outcomes: A Secondary Analysis of the Frequent Hemodialysis Network Trials. Blood Purif 2016;41:277–286.
- Weinhandl, Collins, Kraus. Ultrafiltration Rates with More Frequent Home Hemodialysis. Oral Presentation. 2017 ADC.
- Stefánsson, B.V., Brunelli, S.M., Cabrera, C. et al. Intradialytic hypotension and risk of cardiovascular disease. Clin J Am Soc Nephrol. 2014; 9: 2124–2132.
- Jefferies, H.J., et al. Frequent Hemodialysis Schedules Are Associated with Reduced Levels of Dialysis-induced Cardiac Injury (Myocardial Stunning). Clin J Am Soc Nephrol. 2011 June; 6(6): 1326–1332.
- Jaber BL, Lee Y, Collins AJ, et al. Effect of daily hemodialysis on depressive symptoms and postdialysis recovery time: interim report from the FREEDOM (Following Rehabilitation, Economics and Everyday-Dialysis Outcome Measurements) Study. Am J Kidney Dis. 2010;56(3):531-539.
- Lindsay RM, Heidenheim PA, Nesrallah G, Garg AX, Suri R, Daily Hemodialysis Study Group London Health Sciences Centre. Minutes to recovery after a hemodialysis session: a simple health-related quality of life question that is reliable, valid, and sensitive to change. CJASN. 2006;1(5):952-959.
- Jaber BL, et al. Impact of Short Daily Hemodialysis on Restless Legs Symptoms and Sleep Disturbances. CJASN May 2011 vol. 6 no. 5 1049-1056.
- Finkelstien FO, et al. At-home short daily hemodialysis improves the long-term health-related quality of life. Kidney International (2012) 82, 561–569.
- Kraus, Michael A. et al. Intensive Hemodialysis and Health-Related Quality of Life. Am J of Kidney Dis. 2016;68:S33-S42.
- Hanley, P.J., Pierratos, A. Improvement of sleep apnea in patients with chronic renal failure who undergo nocturnal hemodialysis. N Engl J Med: 2001; Vol. 344, No. 2.
- Daugirdas JT, Chertow GM, Larive B, et al. Effects of frequent hemodialysis on measures of CKD mineral and bone disorder. JASN. 2012;23(4):727-738.
- Copland, M. et al. Intensive Hemodialysis, Mineral and Bone Disorder, and Phosphate Binder Use. Am J Kid D: 2016; Volume 68, Issue 5, Supplement 1, Pages S24–S32.
- Foley, R. N., Gilbertson, D. T., Murray, T., Collins, A. J. Long interdialytic interval and mortality among patients receiving hemodialysis. NEJM. 2011;365(12):1099-1107.
- Assimon, M.M. et al. Ultrafiltration Rate and Mortality in Maintenance Hemodialysis Patients. Am J Kidney Dis. 2016;68(6):911-922.
- Flythe, J.E., Curhan, G.C., Brunelli, S.M. Clin J Disentangling the Ultrafiltration Rate–Mortality Association: The Respective Roles of Session Length and Weight Gain. Clin J Am Soc Nephrol. 2013 Jul;8(7):1151-61.
- Gotch FA. Modeling the Dose of Home Dialysis. Home Hemodial Int, Vol. 3, 37–40, 1999.
- Daugaridas et al; Anthropometrically estimated total body water volumes are larger than modeled urea volume in chronic hemodialysis patients: Effects of age, race and gender. KI 64(2003), 1108 – 1119.
- Daugaridas et al; Standard Kt/V urea: a method of calculation that includes effects of fluid removal and residual renal clearance. KI77(2010), 637 – 644.