What is Nocturnal Dialysis?
Nocturnal Dialysis (sometimes referred to as overnight dialysis), is, simply put, dialysis therapy that is performed overnight while you sleep.
While some dialysis centers offer nocturnal dialysis within the clinic, here we will discuss the two types of nocturnal dialysis therapies available within your home – Home Hemodialysis (HHD) and Automated Peritoneal Dialysis (APD), also known as Continuous Cycling Peritoneal Dialysis (CCPD).
Nocturnal Home Hemodialysis (HHD)
What is Nocturnal HHD?
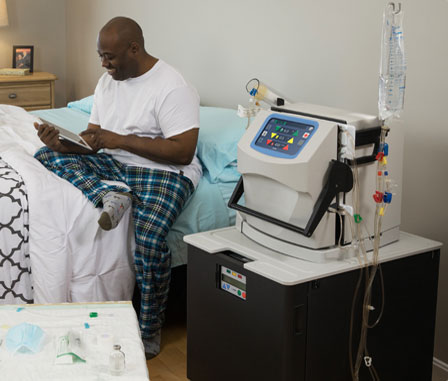
Nocturnal HHD uses a hemodialysis machine in your home to accomplish similar treatment goals as daytime hemodialysis (including removing excess waste and toxins from your blood) but it is done overnight, while you and your care partner are asleep.
The NxStage systems are the only hemodialysis machines in the United States cleared by the FDA for nocturnal home hemodialysis treatments.
What are some of the differences between MORE FREQUENT daytime HHD and nocturnal HHD?
While daytime HHD sessions typically last 3 to 4 hours nocturnal therapy sessions are usually 6-8 hours in duration. Nocturnal HHD treatments are also generally performed 4-6 times per week (all treatment times will vary depending on your prescription).
Fluid and toxin removal with more frequent nocturnal HHD is closer to that of a healthy kidney, which works 24 hours a day, 7 days a week. With these extended treatments, you may experience less toxin and fluid build-up, have shorter post-dialysis recovery time after treatment, and have more energy.
How Might Nocturnal HHD Benefit My Quality-of-Life and Health?
Automated Peritoneal Dialysis (APD)
What is APD?
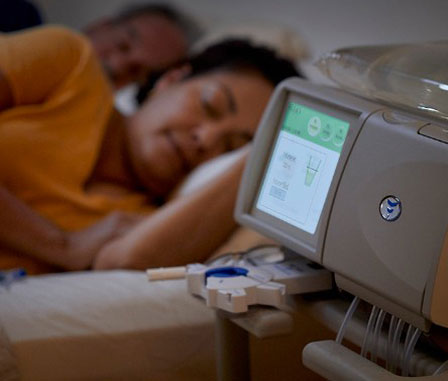
Peritoneal dialysis uses blood vessels in the lining of your peritoneal cavity, called the peritoneum, to filter and clean your blood. When you perform APD, PD solution is infused into your peritoneal (abdominal) cavity using a cycler, overnight while you sleep. The PD solution then absorbs waste, toxins and excess fluid from your blood, which are removed when the dialysate is drained. In the morning, the cycler can leave you dry or do a Last Fill that allows you to also dwell during the day.
What are some of the differences between Continuous Ambulatory Peritoneal Dialysis (CAPD) and APD?
CAPD typically requires a patient to perform 3-5 manual treatments throughout the day. Exchanges last from 20 to 30 minutes each. APD typically takes place over a single, extended treatment period while you sleep, and can negate the need for manual filling and draining.
More about Nocturnal Dialysis
Who is a candidate for nocturnal dialysis?
Ultimately this decision will be made by you and your doctor after discussing your therapy options and the many aspects of performing dialysis. You and your doctor will ensure that you are physically able to administer therapy and that you complete the required training.
Nocturnal HHD requires a care partner to be present during therapy. Both the patient and care partner sleep during therapy. You and your care partner will receive thorough training before transitioning to nocturnal treatments.
Will I be able to sleep during nocturnal dialysis?
Like most shifts in medical treatment, nocturnal dialysis may have an adjustment period. It can take time for your body to adjust to sleeping while performing therapy. Over time, however, many patients are able to sleep comfortably through the night with few complications. For additional considerations see below.
What if my machine alarms?
The training you receive from you nurse will help prepare you to handle common machine alarms at home. In many cases, an alarm can be identified by the patient, and the problem rectified using prompts on your cycler screen and by referencing the user guide. Should you or your care partner need additional assistance, you can call technical or customer support and they will help troubleshoot.
What will I need to start nocturnal dialysis therapy?
Once you have a prescription for therapy and have been trained you will need the following.
For Nocturnal HHD
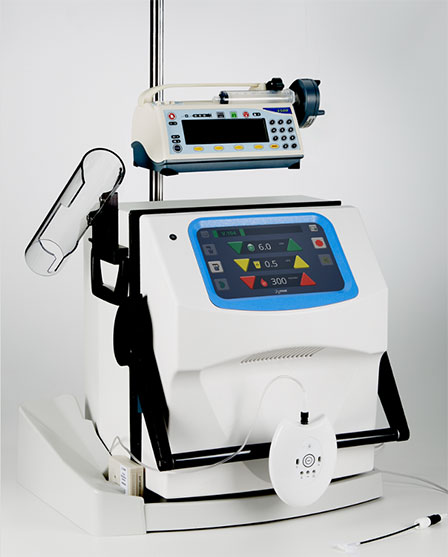
- A NxStage home hemodialysis machine such as the NxStage® VersiHD™ or the NxStage® System One™.
- The applicable user guide and any supplemental instructional materials.
- A venous needle dislodgment device, which alerts you to a vascular access blood leak.
- NxStage fluid detection system – Includes cycler base, extended cycler base, filter holder, and fluid detection sensor. More information on NxStage System Ancillary Devices can be found here.
- An infusion pump, if continuous anticoagulant infusion is desired/required.
- All typical hemodialysis supplies, including cartridges, dialysate, sterilization supplies, bandages, etc.
- A place to store your equipment and supplies. Your care team and/or customer service team can help with suggestions and set-up.
For Nocturnal APD
- An APD machine (cycler), such as the Liberty Select.
- The applicable user guide and any supplemental instructional materials.
- All typical peritoneal dialysis supplies such as PD solution, drain bags or drain lines, cassettes etc.
- A place to store your equipment and supplies. Your care team and/or customer service
team can help with suggestions and set-up.
Transitioning to Nocturnal Dialysis
The decision to do nocturnal home dialysis is a big step and one that requires a discussion with your doctor. Whether you choose nocturnal HHD or nocturnal PD, training is required and there will be adjustments to the time, place, and process of dialyzing. Understandably, some patients are hesitant to change their chosen therapy, as it comes with adjustments, additional training, and a bit of uncertainty. However, nocturnal home dialysis may offer you many clinical and lifestyle benefits over traditional daytime and/or in-center dialysis.
If you and your doctor decide switching to nocturnal dialysis is a good option, you will receive a prescription for the therapy, and you and your care partner (if applicable) will be trained to perform overnight treatments at home. Training includes instruction on setting up and operating the machine, sleeping comfortably and safely while dialyzing, identifying and troubleshooting alarms, and other information unique to home nocturnal HHD process.
If you are new to HHD and are considering nocturnal therapy, speak with your care team about starting more frequent hemodialysis treatments, at home, during the day for a period of time. Once you are comfortable with performing your treatments at home, it is usually possible for you and your care partner to return to the clinic to receive additional training for nocturnal treatments. This usually takes 4-5 additional days and includes education on the following:
- Ancillary equipment use and infusion pump
- Taping methods to secure access needles and lines
- Proper dosing of heparin for anticoagulation
Talk to a Patient Consultant
Risks and Responsibilities
Patients should review the following information carefully and discuss it with their doctors to decide whether home hemodialysis with NxStage systems is right for them.
Users should weigh the risks and benefits of performing home hemodialysis with NxStage systems.
- Medical staff will not be present to respond to health emergencies that might happen during home treatments, including, among other things, dizziness, nausea, low
blood pressure, and fluid or blood leaks. - Users may not experience the reported benefits of home, more frequent, or nocturnal hemodialysis with the NxStage systems.
- The NxStage systems require a prescription for use.
Users will be responsible for all aspects of their hemodialysis treatment from start to finish.
- Medical staff will not be present to perform home treatments. Users will be responsible for, among other things, equipment setup, needle insertions, responding to and resolving system alarms, system tear-down after treatment, monitoring blood pressure, ensuring proper aseptic technique is followed, and following all the training material and instructions that nurses provide.
Users will need additional resources to perform home hemodialysis.
- Users will need a trained care partner to be present during your treatment at home (unless their doctor prescribes “solo/independent” home hemodialysis, described below).
- Users must have a clean and safe environment for their home treatments.
- Users will need space in their home for boxes of supplies necessary to perform home hemodialysis with NxStage systems.
Certain forms of home hemodialysis have additional risks.
- If a doctor prescribes home hemodialysis more than 3 times a week, vascular access is exposed to more frequent use which may lead to access related complications, including infection of the site. Doctors should evaluate the medical necessity of more frequent treatments and discuss the risks and benefits of more frequent therapy with users.
- If a doctor prescribes “solo/independent” home hemodialysis without a care partner during the day, risks of significant injury or death increase because no one is present to help users respond to health emergencies. If users experience needles coming out, blood loss, or very low blood pressure during solo/independent home hemodialysis, they may lose consciousness or become physically unable to correct the health emergency. Users will need additional ancillary devices and training to perform solo/independent home hemodialysis.
- If a doctor prescribes “nocturnal” home hemodialysis at night while the user and a care partner are sleeping, risks increase due to the length of treatment time and because therapy is performed while the user and a care partner are sleeping. These risks include, among other things, blood access disconnects and blood loss during sleep, blood clotting due to slower blood flow or increased treatment time or both, and delayed response to alarms when waking from sleep. A doctor may need to adjust users’ medications for nocturnal home hemodialysis, including, among other things, iron, Erythropoiesis-Stimulating Agents (ESA), insulin/oral hypoglycemics, anticoagulants, and phosphate binders.
The reported benefits of peritoneal dialysis may not be experienced by all patients.
Peritoneal dialysis does involve some risks that may be related to the patient, center, or equipment. These include, but are not limited to, infectious complications. Examples of infectious complications include peritonitis and exit-site and tunnel infections. Non-infectious complications include catheter complication such as migration and obstruction, peritoneal leaks, constipation, hemoperitoneum, hydrothorax, increased intraperitoneal volume, and respiratory and gastric issues. It is important for healthcare providers to monitor patient prescriptions and achievement of adequate fluid management goals.
Patients should consult their doctor to understand the risks and responsibilities of performing peritoneal dialysis.
References:
- Heidenheim PA, Muirhead N, Moist L, Lindsay RM. Patient quality of life on quotidian hemodialysis. Am J Kidney Dis. 2003;42(S1)(S1):S36-S41.
- Daugirdas, John T.; Blake, Peter G.; and Ing, Todd S., "Handbook of Dialysis (5th ed.)" (2015).
- Lindsay RM, Heidenheim PA, Nesrallah G, Garg AX, Suri R, Daily Hemodialysis Study Group London Health Sciences Centre. Minutes to recovery after a hemodialysis session: a simple health-related quality of life question that is reliable, valid, and sensitive to change. CJASN. 2006;1(5):952-959. doi:10.2215/CJN.00040106.
- Pauly, R. P., Gill, J. S., Rose, C. L., Asad, R. A., Chery, A., Pierratos, A., & Chan, C. T. (2009). Survival among nocturnal home haemodialysis patients compared to kidney transplant recipients. Nephrology Dialysis Transplantation, 24(9), 2915–2919. https://doi.org/10.1093/ndt/gfp295
- McCullough, P. A., Chan, C. T., Weinhandl, E. D., Burkart, J. M., & Bakris, G. L. (2016). Intensive Hemodialysis, Left Ventricular Hypertrophy, and Cardiovascular Disease. American Journal of Kidney Diseases, 68(5), S5–S14. https://doi.org/10.1053/j.ajkd.2016.05.025
- Bakris, G. L., Burkart, J. M., Weinhandl, E. D., McCullough, P. A., & Kraus, M. A. (2016). Intensive Hemodialysis, Blood Pressure, and Antihypertensive Medication Use. American Journal of Kidney Diseases, 68(5), S15–S23. https://doi.org/10.1053/j.ajkd.2016.05.026
- Culleton BF, Walsh M, Klarenbach SW, et al. Effect of frequent nocturnal hemodialysis vs conventional hemodialysis on left ventricular mass and quality of life: a randomized controlled trial. JAMA. 2007;298(11):1291-1299. doi:10.1001/jama.298.11.1291.